Introduction
Most people who get diagnosed with a hiatus hernia surgery required are told the same thing. Manage your diet. Take your antacids. See how it goes. And often that works. It genuinely does. Lifestyle changes and medication control the symptoms for a large percentage of people, sometimes indefinitely.
They live with the hernia the way you live with a creaky floorboard — aware of it, mildly annoyed by it, but mostly fine. But then there’s the other group. Many patients eventually ask when hiatus hernia surgery required, especially when symptoms start affecting daily life despite medication. Understanding when hiatus hernia surgery required helps patients make informed decisions about treatment options.
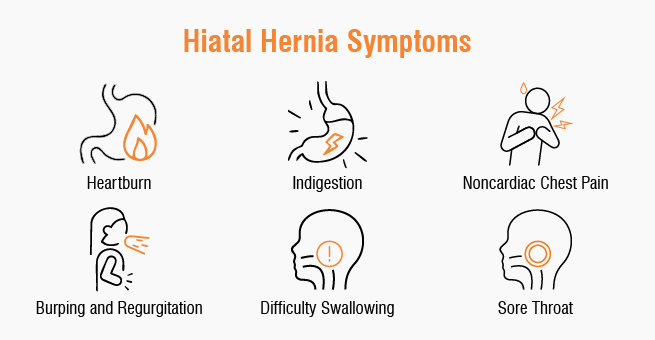
The ones for whom it keeps getting worse. Whose medication stops working properly. Whose symptoms bleed into sleep, into work, into the ordinary texture of everyday life. Who stand in a doctor’s office eventually asking — does this need surgery? That’s what this is about. When hiatus hernia surgery becomes the answer. And why.
If you’re unsure about your condition, it’s important to understand hiatus hernia causes, symptoms and when to see a doctor before considering treatment options.
Hiatus hernia surgery is required when symptoms like severe acid reflux, difficulty swallowing, or regurgitation do not respond to medication and lifestyle changes. Surgery is also recommended in large hernias or when complications such as Barrett’s esophagus or aspiration occur.
When Is Hiatus Hernia Surgery Required for Most Patients
Not all patients hiatus hernia surgery required, as many cases are managed with lifestyle changes and medication.Most patients wonder when hiatus hernia surgery required, but the answer depends on symptom severity and response to treatment. Start here because it’s important.
The majority of hiatus hernias — the sliding kind, which accounts for most cases — are managed conservatively. Medications like proton pump inhibitors (omeprazole, pantoprazole) reduce acid production.
Dietary changes reduce reflux episodes. Elevating the head of the bed helps at night. For a large number of people this is enough. Surgery is not the default. It’s not even the second step for most.
The conversation about symptomatic hernia treatment almost always starts with lifestyle and medication, sometimes for years before surgery enters the picture. So if you’ve just been diagnosed — breathe. Surgery is not automatically in your future. Doctors usually recommend hiatus hernia surgery required only when conservative treatment fails.
Many patients manage symptoms effectively by following a proper hiatus hernia diet with foods to eat and avoid.
When Symptoms Start Demanding More
One of the main reasons for considering hiatus hernia surgery is worsening or uncontrolled symptoms.The clearest signal that hiatus hernia surgery might be needed is when symptoms stop responding to treatment that was previously working.
This is a pattern worth tracking. If you’re on your second or third medication adjustment in a year, if the dosage keeps going up, if you’re taking antacids multiple times a day on top of prescription medication — that escalation is data.
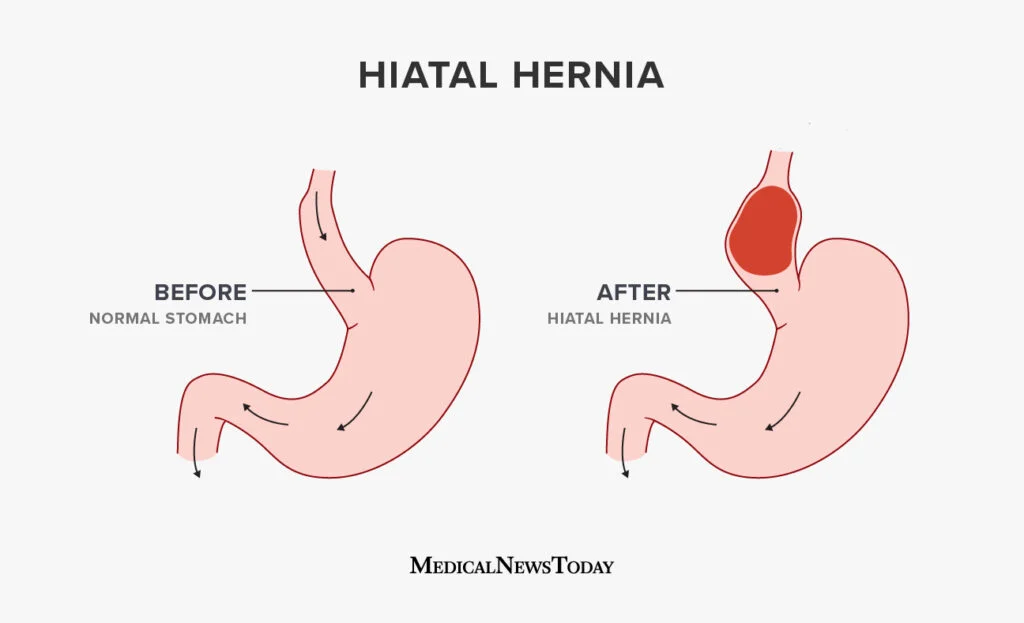
It tells you the hernia is either worsening or your body is simply not getting adequate relief from pharmaceutical management. Specific symptoms that tend to push the conversation toward surgery:
• Severe, persistent acid reflux that isn’t controlled by maximum medication doses
• Regurgitation — actual food or liquid coming back up — that is happening frequently, affecting meals, and impacting quality of life
• Difficulty swallowing (dysphagia), which can indicate the hernia is creating structural pressure on the esophagus
• Chronic chest pain or discomfort that has been thoroughly investigated and is attributed to the hernia
• Recurrent aspiration — stomach contents entering the lungs — which can cause respiratory problems including pneumonia
• Significant Barrett’s esophagus developing as a consequence of long-term, uncontrolled reflux
These symptoms often indicate the need for hiatus hernia surgery.
Each of these represents a point where the risk calculation shifts. Where the risks of not operating begin to outweigh the risks of the surgery itself.
If symptoms persist despite following a hiatus hernia diet plan, further treatment may be required.
Hernia Size and Type Matter
The need for hiatus hernia surgery also depends on the size and type of hernia. Not all hiatus hernias behave the same way and hernia progression is one of the factors surgeons track carefully. A small sliding hiatus hernia in an otherwise healthy person is a very different clinical picture than a large paraesophageal hernia where a significant portion of the stomach has migrated into the chest.
The latter carries genuine risks — including the possibility of gastric volvulus, where the stomach twists on itself, which is a surgical emergency. Paraesophageal hernias are treated differently. Because of their anatomy and the risk profile, many surgeons recommend repair even when symptoms are relatively mild, particularly in patients who are younger and healthy enough to tolerate surgery well.
The logic being — better to fix it before an emergency than after. Sliding hernias are more typically managed conservatively unless symptoms are severe. Larger or paraesophageal hernias are more likely to require hiatus hernia surgery.
In such cases, choosing the best hospital for laparoscopic surgery in Hisar becomes important for safe treatment.
When Surgery Becomes the Recommendation
Doctors recommend hiatus hernia surgery in specific clinical situations where long-term relief is needed. There are several clinical scenarios where the decision tips toward surgery. Understanding them helps make sense of what your doctor may be recommending. Medication dependence with inadequate control — being on high-dose PPIs long-term is not without its own concerns. Long-term PPI use is associated with effects on bone density, magnesium absorption, and in some research, kidney function. If someone needs high-dose medication indefinitely to maintain only partial control, surgery as a one-time solution becomes genuinely attractive.
Young patients — a 35-year-old with a significant hernia faces potentially decades of medication. Surgery at that age carries lower risk and the long-term benefit calculus is different than for a 70-year-old. Preference for a definitive solution — some patients, after understanding the options, simply prefer the surgery. They want to eat normally. They want to sleep without elevating their head. They want to stop taking daily medication. That’s a legitimate reason and most surgeons will take it seriously. Failed previous procedures — if someone has had a prior surgery that has failed or produced a recurrence, surgical revision becomes necessary. In such cases, hiatus hernia surgery required provides a more permanent solution.
What the Surgery Actually Is
Hiatus hernia surgery required is usually performed using a laparoscopic technique called fundoplication. The standard surgical approach is a laparoscopic fundoplication — most commonly a Nissen fundoplication. The surgeon wraps the upper part of the stomach around the lower esophagus, creating a new valve mechanism that prevents reflux. The hernia is also repaired by closing the hiatal opening. Laparoscopic means small incisions, shorter hospital stay, faster recovery compared to open surgery. Most patients go home in one to two days. Return to normal activity within a few weeks. It works well. Long-term studies show high satisfaction rates.
The majority of patients report significant improvement or complete resolution of reflux symptoms. Some patients develop temporary or persistent difficulty with belching or swallowing — this is a known trade-off and worth discussing with your surgeon. For complex cases — large paraesophageal hernias, revision surgeries — the procedure is more involved and recovery is longer. But the fundamentals are the same. Most patients experience significant improvement after hiatus hernia surgery required.
The Honest Answer to ‘Do I Need Surgery’
The decision for hiatus hernia surgery required depends on symptoms, response to treatment, and overall health.
It depends on four things. How severe your symptoms are. How well they’re controlled with current symptomatic hernia treatment. How the hernia is behaving structurally — its size, type, any signs of hernia progression. And your personal circumstances — age, overall health, how much the symptoms are affecting your life. There isn’t a bright line that everyone crosses at the same moment. This is a conversation between you and a specialist, ideally a gastroenterologist and a surgeon together, looking at your specific situation.
What you should walk away from that conversation with is: a clear understanding of your hernia type and size, an honest assessment of how well current management is working, and if surgery is being recommended — why specifically, what it involves, and what outcomes you can realistically expect. Ask those questions. Insist on answers. A specialist can help determine whether hiatus hernia surgery required is the right option.
Conclusion
Hiatus hernia surgery required is recommended when symptoms become severe or unmanageable with medication. For many patients, hiatus hernia surgery required offers long-term relief and improved quality of life. It’s just a different clinical scenario — one where the hernia has either grown to a point where it’s structurally risky, or where symptoms have genuinely run out of road with conservative treatment.
Surgery in these cases is not a last resort. It’s a well-established, highly effective option that for many patients ends years of discomfort in a single procedure. If you’re being told you need hiatus hernia surgery — get the full picture. Understand what you’re dealing with. And then make a decision with your medical team that you actually understand and are at peace with.
Frequently Asked Questions
Q1. Can a hiatus hernia heal on its own without surgery?
Hiatus hernias don’t heal spontaneously — the structural displacement of stomach tissue through the diaphragm doesn’t reverse without intervention. However, symptoms can be very well controlled with diet, lifestyle, and medication for many years or indefinitely, meaning many people never need surgery.
Q2. What happens if hiatus hernia surgery is delayed?
For sliding hernias, delay is often acceptable with proper management. For large paraesophageal hernias, delay carries some risk of serious complications including gastric volvulus. Your surgeon will guide you on urgency based on your specific hernia type.
Q3. How do I know if my hiatus hernia is getting worse?
Signs of hernia progression include worsening reflux that requires increasing medication, new symptoms like difficulty swallowing, more frequent regurgitation, or symptoms extending to the respiratory system (coughing, hoarseness). An endoscopy or barium swallow study can assess structural changes.
Q4. Is laparoscopic hiatus hernia surgery safe?
Laparoscopic fundoplication is a well-established procedure with a strong safety record. Complication rates are low in experienced hands. The most common long-term issue is some difficulty belching or occasional bloating — outcomes that most patients find acceptable given the relief from reflux.
Q5. How long does recovery from hiatus hernia surgery take?
Most patients return home one to two days after laparoscopic surgery. A soft diet is required for several weeks as the wrap heals. Most people return to desk work within two to three weeks and full physical activity within four to six weeks.


