Introduction
Understanding hernia vs acid reflux is important because both conditions can cause similar symptoms like chest burning, stomach pain, and discomfort after meals, making it difficult to identify the exact issue without proper evaluation.
The feeling after a meal that something isn’t right — but you can’t quite tell what or where. Is it a hernia? Is it reflux? Is it both? And does the answer even matter if the symptoms feel the same? It matters quite a bit, actually. Because a hernia is a structural problem and reflux is a chemical one, and while they frequently coexist, they can also exist independently — and treating one without addressing the other leaves you in exactly the same uncomfortable place.
This is the breakdown. Hernia vs acid reflux — what each actually is, how the symptoms differ, where they overlap, and how you figure out which one you’re dealing with.
Hernia vs acid reflux are two different conditions that often show similar symptoms like heartburn and chest pain. Acid reflux (GERD) is a functional issue caused by stomach acid flowing back into the esophagus, while a hernia is a structural problem where part of the stomach pushes through the diaphragm. Although both conditions can coexist, proper diagnosis through tests like endoscopy is important to determine the correct treatment. Managing lifestyle, diet, and medical care plays a key role in controlling both conditions effectively.
Hernia vs Acid Reflux: What’s the Real Difference?
To understand hernia vs acid reflux, it is important to know how acid reflux works inside the body.
Acid reflux happens when stomach acid travels back up through the lower esophageal sphincter — the valve that’s supposed to keep stomach contents going in one direction — and irritates the lining of the esophagus. When this happens frequently enough, it becomes GERD: Gastroesophageal Reflux Disease. GERD is a functional problem. The valve isn’t working properly.
This can happen for lots of reasons — diet, obesity, pregnancy, certain medications, stress, and yes, hiatus hernia. GERD doesn’t require a structural abnormality to exist. Many people have severe reflux with no hernia at all. GERD vs hernia symptoms can look identical at first glance. Both cause heartburn. Both cause regurgitation. Both can cause chest discomfort that mimics cardiac pain. The difference is in the structural picture underneath the symptoms.
What Is a Hiatus Hernia?
In the discussion of hernia vs acid reflux, a hiatus hernia represents the structural side of the problem.
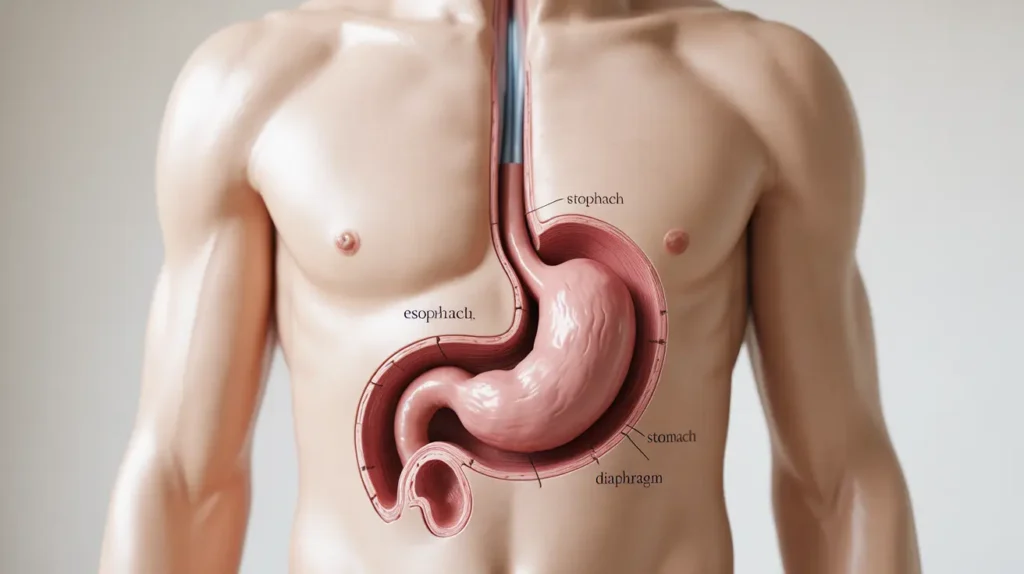
A hiatus hernia is when part of the stomach pushes upward through the diaphragm — the muscle separating the chest from the abdomen — into the chest cavity. This is structural. Something has physically moved that shouldn’t have. And because the stomach is now partly in the wrong place, the lower esophageal sphincter — which sits at the junction — gets disrupted.
This is why hiatus hernias so commonly cause reflux. The structural displacement undermines the valve’s function. But here’s the nuance that matters: not every hiatus hernia causes symptoms. Some hernias are found incidentally on scans done for completely unrelated reasons. And hernia vs acid reflux isn’t always an either/or — in many patients, the hernia is causing or worsening the reflux, and both need to be considered in treatment.
How the Symptoms Differ
When comparing hernia vs acid reflux, symptoms often overlap, making diagnosis challenging.
There are some distinguishing characteristics, though they aren’t absolute. When evaluating GERD vs hernia symptoms, these patterns can help:
Symptoms more typical of reflux / GERD alone:
• Burning sensation in the chest (heartburn) — typically after meals or when lying down
• Sour or bitter taste at the back of the mouth
• Chronic cough, particularly at night
• Hoarseness in the morning — acid irritating the vocal cords
• Symptoms that respond well to antacids or PPIs
Symptoms that may suggest a hernia component:
• Sensation of fullness or pressure in the chest or upper abdomen, not just burning
• Difficulty swallowing — because the hernia may create a mechanical obstruction
• Chest pain that feels positional — worse in certain body positions
• Reflux symptoms that are severe and don’t respond normally to medication — suggesting the structural issue is undermining treatment
• Symptoms that are worse after large meals and better after small ones — reflecting the stomach volume-pressure relationship
The honest answer is that stomach pain and chest discomfort from both conditions can feel functionally identical. Clinical examination, endoscopy, and imaging are what actually distinguish them — not symptom pattern alone.
The Overlap Problem
Here’s where hernia vs acid reflux Hisar gets complicated in practice. Most people with a significant hiatus hernia have reflux. Most people with severe reflux are checked for a hernia at some point. The conditions share mechanisms. The treatments partially overlap — dietary modification helps both, PPIs help both.
But if you only treat the reflux and don’t address the hernia, you may be chasing symptoms indefinitely. And if you address the hernia surgically without acknowledging the reflux-triggering dietary patterns, you may find symptoms returning faster than expected. A good clinician treats both as part of the same picture.
When to Investigate
Certain symptoms should prompt investigation sooner rather than later:
• Difficulty swallowing — always investigate. This is not a wait-and-see symptom
• Unintentional weight loss alongside digestive symptoms
• Stomach pain that’s different from usual — new character, new location, more severe
• Symptoms that don’t respond to standard reflux treatment after four to eight weeks
• Vomiting blood or dark stools — emergency investigation
If symptoms do not improve or become severe, it is important to understand when is hiatus hernia surgery required for proper diagnosis and treatment.
The standard investigations are an upper endoscopy (which visualizes the esophagus and stomach directly) and sometimes a barium swallow study (which shows the structural anatomy under X-ray). These two tests together will usually give a clear answer on both the reflux picture and whether a hernia is present.
Treatment Differences
Understanding hernia vs acid reflux is crucial because treatment approaches for both conditions are different.
This is where the distinction matters most practically. GERD without a hernia is treated with PPIs, dietary changes, and lifestyle modification. A hiatus hernia producing symptoms follows the same first steps — but if symptoms are severe or not responding, surgery addresses the structural problem in a way that medication simply cannot.
Treating pure reflux with surgery when there is no structural hernia present is rarely indicated. Treating a large symptomatic hernia with medication alone may be perpetually inadequate.
Understanding which one you have — or whether you have both — shapes the treatment path significantly.
For cases where a structural issue like hernia is involved, advanced procedures such as laparoscopic surgery can provide effective long-term relief. You can learn more about this in detail here.
Conclusion
In conclusion, understanding hernia vs acid reflux helps in identifying the root cause of symptoms and choosing the right treatment approach.
The answer to hernia vs acid reflux isn’t always clean. These conditions overlap, coexist, and sometimes masquerade as each other. What they don’t do is self-diagnose. If you’re in Hisar or anywhere else dealing with chronic heartburn, persistent stomach pain, or symptoms that aren’t resolving — get an endoscopy. It’s the most direct way to see what’s actually happening. The distinction between GERD vs hernia symptoms in clinical practice comes from seeing, not guessing. Know what you’re dealing with. Treatment becomes much clearer from there.
Frequently Asked Questions
Q1. Can you have both a hernia and acid reflux at the same time?
Yes — very commonly. A hiatus hernia often causes or worsens acid reflux because the structural displacement of the stomach disrupts the valve that prevents acid from traveling upward. Managing both conditions together is the most effective approach.
Q2. How do I know if my chest pain is from a hernia or reflux?
Clinically, it’s difficult to distinguish purely from symptoms. Both conditions can cause chest pain, burning, and discomfort. Positional pain, difficulty swallowing, or pain that doesn’t respond well to antacids may suggest a hernia component. An endoscopy provides definitive information.
Q3. Can GERD cause a hiatus hernia?
Long-term severe GERD doesn’t directly cause a hiatus hernia, but the two are strongly associated. Factors that cause reflux — obesity, chronic straining, certain medications — can also contribute to hernia formation over time.
Q4. Is acid reflux always present with a hiatus hernia?
No. Some hiatus hernias, particularly small sliding ones, are asymptomatic and found incidentally. Not every hernia produces reflux. The size, type, and position of the hernia influence whether and how much it disrupts valve function.
Q5. What tests confirm a hiatus hernia vs acid reflux?
Upper endoscopy is the most commonly used investigation — it visualizes the esophagus, stomach, and junction directly. A barium swallow study provides anatomical information about the hernia. pH monitoring measures actual acid levels in the esophagus over time, useful for quantifying reflux severity


