Introduction
People arrive at the laparoscopy conversation carrying things they’ve heard. From relatives. From the internet. From a neighbor whose cousin had a bad experience. From half-remembered articles and old advice that may or may not have been accurate when it was given. Some of what they carry is accurate.
A lot of it isn’t. Laparoscopy surgery myths are persistent in a way that genuinely affects decisions — people delay necessary procedures, refuse investigations, or arrive anxious and misinformed about what they’re actually signing up for. Let’s go through the five that come up most often. Not to dismiss concerns — some concerns about surgery are entirely valid — but to separate what’s real from what isn’t. These common laparoscopy surgery myths often create confusion among patients
Laparoscopy surgery myths often create confusion about safety, recovery time, and effectiveness. In reality, laparoscopic procedures are safe, minimally invasive, and offer faster recovery compared to open surgery. Understanding these myths helps patients make informed decisions and reduces unnecessary fear.
Myth 1: Top Laparoscopy Surgery Myths You Should Stop Believing
This is probably the most common surgery misconception in this space. The thinking goes: smaller incisions, less intervention, therefore less thorough, therefore less reliable. The reality is more or less the opposite. Laparoscopic surgery provides surgeons with a magnified, high-definition camera view of the operative field — often better than what’s visible to the naked eye during open surgery.
The precision of instrument work in laparoscopy is extremely high. For procedures like cholecystectomy (gallbladder removal), hernia repair, appendectomy, and antireflux surgery, hernia repair, appendectomy, and antireflux surgery. If you’re unsure about treatment decisions, you can also read about when hiatus hernia surgery is required outcomes in laparoscopic procedures are equivalent to or better than open surgery, with substantially lower complication rates.
The technique is different. The effectiveness is not lesser. There are specific situations where open surgery is still preferred or necessary — very complex adhesions, certain emergency scenarios, cases where laparoscopic view is inadequate. But ‘less effective’ is not a reason. This clearly proves that many laparoscopy surgery myths are misleading
Myth 2: Laparoscopic Surgery Is Too Risky
The safety concerns around laparoscopy surgery myths are understandable — it is surgery, and surgery carries risk. But ‘laparoscopy is too risky’ as a general statement is not supported by evidence. All surgery carries risk. The relevant question is always: how do the risks of this procedure compare to the risks of not doing it? For most elective laparoscopic procedures — hernia repair, gallbladder removal, diagnostic laparoscopy — the complication rates are low.
Serious complications like bowel injury, major bleeding, or anaesthetic reactions exist but are uncommon in experienced hands. The complication rate for laparoscopic procedures is generally lower than for equivalent open procedures, because smaller incisions mean less tissue trauma, lower infection risk, and faster healing. The risk is real. It is not the reason most people imagine it to be. Such beliefs are part of common laparoscopy surgery myths.
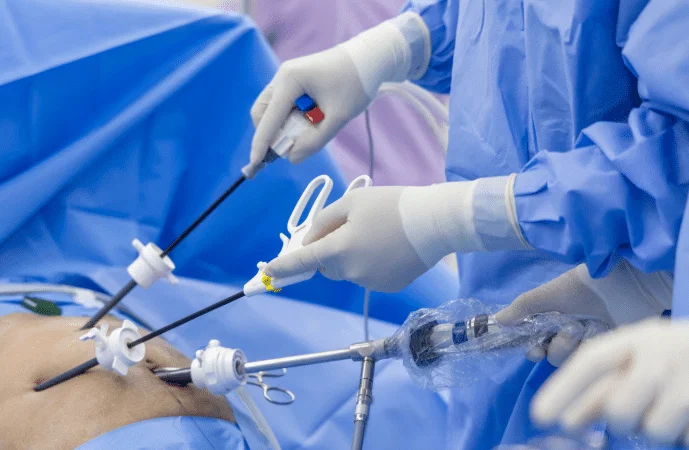
Myth 3: Recovery Takes Months
This laparoscopy surgery myth is particularly damaging because it causes people to delay procedures unnecessarily, calculating that they simply don’t have months to be out of commission. The actual recovery timeline for standard laparoscopic procedures: Most patients are home within one to two days. Most return to light work within one to two weeks.
Most return to full normal activity within four to six weeks. Most return to full normal activity within four to six weeks. During recovery, following the right diet is also important — you can check hiatus hernia diet foods to eat and avoid for better healing. Some straightforward procedures — like diagnostic laparoscopy or minor adhesion release — have even shorter recoveries.
The months-long recovery picture comes from open surgery. laparoscopy surgery myths was developed precisely because it dramatically reduced recovery time. The whole point of the smaller incisions is faster healing — less muscle cutting, less tissue trauma, less post-operative pain, and therefore faster mobilisation. If someone told you laparoscopy takes months — they were either describing open surgery or a particularly complex procedure. Standard laparoscopy is measured in weeks. This misunderstanding comes from outdated laparoscopy surgery myths.
Myth 4: The Gas Used in Laparoscopy Is Dangerous
This one comes up with surprising frequency among patients who have read a little about the procedure. Carbon dioxide is used to inflate the abdomen during laparoscopy surgery myths , creating the working space the surgeon needs. And CO2, given that it’s associated with environmental concerns and suffocation in high concentrations, sounds alarming when you hear it’s being pumped into your body. But CO2 is actually chosen specifically because it’s safe. It’s rapidly absorbed by the body.
It’s cleared through normal breathing within hours. It doesn’t support combustion (important given that electrosurgical instruments are used during laparoscopy). And it’s physiologically inert at the concentrations used. The shoulder pain that many patients experience post-operatively is caused by residual CO2 irritating the diaphragm — but this resolves within 24-72 hours and is not dangerous.
This particular surgery misconceptiondoesn’t have a strong basis in physiology once you understand what CO2 actually does in the body. This concern is one of the most misunderstood laparoscopy surgery myths.
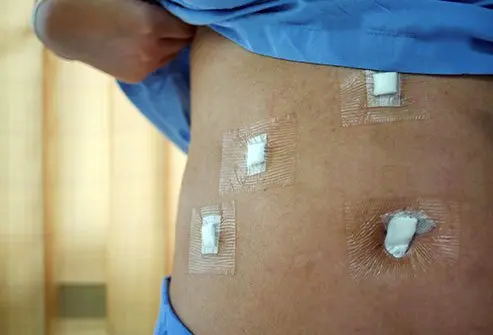
Myth 5: Laparoscopic Surgery Leaves Big Scars
The opposite is true, and it’s actually one of the most significant advantages of the technique. Laparoscopic incisions are typically 0.5 to 1 centimetre — smaller than your thumbnail. Most procedures require three to four such incisions. These heal to small, pale marks that fade significantly over time and are often barely visible after a year.
Open surgery for the equivalent procedures would require incisions of ten to thirty centimetres, depending on the operation. The scarring from open surgery is substantial and permanent in comparison. This laparoscopy surgery myth possibly persists because people conflate the emotional weight of surgery with physical marks — it was a big deal, therefore there must be big scars.
The logic is understandable but the correlation doesn’t hold. Small incisions were the design goal. The scars reflect that. This is why such claims are false laparoscopy surgery myths.
What Concerns About Laparoscopy Are Actually Valid?
Because not everything is a myth. Some safety concernsaround laparoscopy deserve honest acknowledgment: Surgeon experience genuinely matters. Laparoscopy has a steeper learning curve than open surgery. Outcomes are better in experienced, higher-volume centres.
If you’re in Hisar or a smaller city, it’s worth asking about your surgeon’s specific experience with your procedure — not to alarm yourself, but to make an informed choice. Conversion to open surgery is possible. Occasionally during a laparoscopic procedure, the surgeon encounters something that requires switching to open. This isn’t a failure — it’s a safety decision. But it does mean recovery changes significantly. Understanding this possibility beforehand is reasonable.
Not all conditions are amenable to laparoscopy. Some complex situations are better handled with open approaches. A good surgeon will tell you this candidly. Not all concerns are myths, but many still fall under laparoscopy surgery myths.
Conclusion
Laparoscopic surgery has been refined over three decades. It is not experimental. It is not inferior. And it is not as risky or recovery-heavy as the myths suggest. The laparoscopy surgery myths misconceptions that persist around it cost people — delay necessary care, add anxiety to already difficult decisions, and sometimes lead people toward less optimal choices based on inaccurate information. Ask questions. Get second opinions if you need them. But base your understanding on what laparoscopy actually is — not what it’s rumoured to be.
Frequently Asked Questions
Q1. Is laparoscopic surgery suitable for everyone?
Most patients are suitable candidates for laparoscopic procedures. Exceptions include patients with very complex previous abdominal surgeries creating dense adhesions, certain cardiac or respiratory conditions that make pneumoperitoneum (abdominal gas inflation) unsafe, or cases where the anatomy makes laparoscopic work technically inadequate.
Q2. How do I choose a good laparoscopic surgeon?
Look for a surgeon with specific training in laparoscopic techniques and a meaningful volume of cases in your specific procedure. Board certification, hospital affiliation, and willingness to discuss their complication rates are all good indicators. Referrals from trusted physicians or from patients who have had the procedure are valuable.
Q3. Can laparoscopy miss something that open surgery would catch?
In experienced hands, the magnified camera view in laparoscopy often provides excellent visualisation. However, tactile feedback — the ability to feel tissue directly — is reduced compared to open surgery. For certain diagnostic situations, open surgery may still provide advantages. This is procedure and situation dependent.
Q4. What is the difference between laparoscopy and laparotomy?
Laparoscopy uses small incisions and a camera. Laparotomy is open abdominal surgery requiring a large incision. Both can accomplish similar goals in many situations, but laparoscopy generally has lower complication rates, less post-operative pain, and faster recovery for equivalent procedures.
Q5. Does laparoscopic surgery hurt more or less than open surgery?
Post-operative pain is generally significantly less with laparoscopic surgery compared to open surgery. Smaller incisions mean less muscle cutting and tissue trauma. Most laparoscopic patients require less pain medication and mobilise faster. The shoulder pain from CO2 gas is the main distinctive discomfort, and it resolves quickly.


